Milestone reached in transplantation research
An international team of researchers, that includes scientists from the German Primate Center (DPZ), has completed a successful transplantation study of porcine insulin-producing islets in rhesus monkeys. The islets, taken from porcine pancreas, are enclosed in a capsule that serves as a bioreactor. This prevents rejection reactions of the immune system. The study was conducted under the leadership of Barbara Ludwig, Stefan Ludwig and Stefan R. Bornstein of the University Hospital Carl Gustav Carus in Dresden. In cooperation with the Israeli company Beta-O2 Technologies Ltd, the researchers developed the artificial pancreatic islet apparatus that has the ability to produce insulin. The transplants were performed at the German Primate Center. After six months, the donor cells produced sufficient insulin and were still intact. The study provides new cell-based treatment options for diabetic patients (PNAS).
The autoimmune disease, diabetes mellitus type 1 is triggered by the destruction of insulin-producing islets. The reason for this occurrence remains a mystery. The lack of insulin leads to permanent hyperglycemia that can lead to numerous secondary diseases such as cardiovascular disease, kidney and nerve damage. According to the Robert Koch Institute, about eight million people are currently suffering from diabetes in Germany. Approximately 400,000 suffer from type 1 diabetes and must provide the body with insulin for the rest of their lives.
The transplantation of human islets for the treatment of type 1 diabetes is currently limited and therefore reserved for high-risk patients where the disease has taken a turn for the worst. Both the lifelong administration of drugs that suppress the immune system (immunosuppressant) and the lack of suitable donor cells, limit the implementation of this method.
Small but highly effective bioreactor
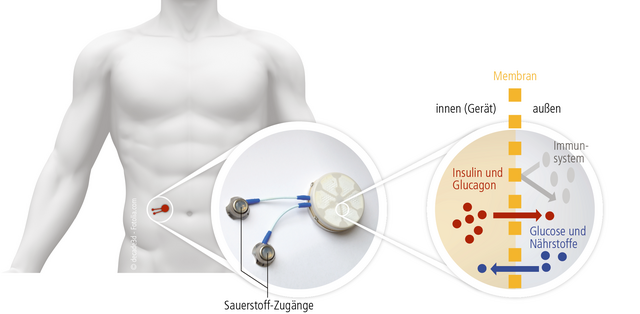
To counteract this condition, scientists from Dresden developed a new strategy to allow for the permanent survival of porcine islets in a capsule. A membrane separated the islets from the rest of the body. Oxygen, glucose and nutrients that are vital for cell survival are able to enter the system and insulin is then transferred to the body. However, certain immune system cells that could damage the islets are not allowed to pass through the membrane. The addition of immunosuppression is therefore superfluous.
The transplantation of the small bioreactor with the islets, occurred at the DPZ. "We prepared the animals for the operations and were also responsible for their aftercare," says Uwe Schönmann, colony manager of the DPZ Primate Husbandry. "The artificial organs showed promising results in the monkeys and produced insulin as soon as the blood sugar levels increased. We did not observe any serious side-effects. It is now time to investigate the effects of the xenografts on humans. „In addition to Schönmann, the DPZ veterinarians Yvonne Knauf and Martina Bleyer were also involved in the study. Franz-Josef Kaup, Head of the Pathology Unit and Primate Husbandry is the project leader at the DPZ.
"Before the transplantation of xenografts are allowed in sick people, the methods must be tested in suitable animal models," says Kaup. "Safety- and feasibility studies with non-human primates are therefore indispensable in the run-up to clinical trials."
In the next step the Paul-Ehrlich-Institute, the German Federal Institute for Vaccines and Biomedicines, will examine the study’s applicability to humans. If clinical trials are allowed in the next few years, the bioreactor could help patients and thereby reduce or even eliminate insulin administration.
The Research Association SFB – Transregio 127
The study was conducted within the framework of the Transregio-Special Research Field (TRR) 127. Since 2012, numerous xenotransplantation experts have been working together in the DFG-funded research network. Scientists are investigating alternative replacement procedures for organs, tissues or cells from pigs. The DPZ plays a pivotal role in this because it provides the recipient animals, give advice to the project partners with their expertise in dealing with non-human primates and provide information on animal welfare issues.
Original publication
Ludwig B, Ludwig S, Steffen A, Knauf Y, Zimmermann B, Heinke S, Lehmann S, Schubert U, Schmid J, Bleyer M, Schönmann U, Colton C, Bonifacio E, Solimena M, Reichel A, Schally A, Rotem A, Barkai U, Grinberg-Rashi H, Kaup FJ, Avni Y, Jones P, Bornstein SR (2017): Favorable outcome of experimental islet xenotransplantation without immunosuppression in a nonhuman primate model of diabetes. PNAS, Proceedings of the National Academy of Sciences, doi: 10.1073/pnas.1708420114